WÜRZBURG.- Previously, it was believed that a germ-free environment was the most critical factor in preventing postoperative infections. However, a recent study by Mercedes Gomez de Agüero's team from the
Max Planck Research Group for Systems Immunology in Würzburg, Germany, in collaboration with the University Hospital of Bern, Switzerland, has revealed that the source of the danger is apparently entirely different: the patients' intestines.
Hospitals have traditionally sought to prevent infections after surgical procedures by maintaining a germ-free environment. It has long been established that concomitant infections during invasive procedures increase mortality rates. For this reason, extensive sterilization measures are implemented to eliminate microorganisms during surgery.
The research team's study shows that the causative agents of these infections have a microbial signature from the intestine. In nearly all patients, the pathogens were intestinal bacteria such as Enterococcus, Escherichia coli, and Clostridium. The research team analyzed the microorganisms that caused concomitant infections in almost 4,000 patients after major surgery.
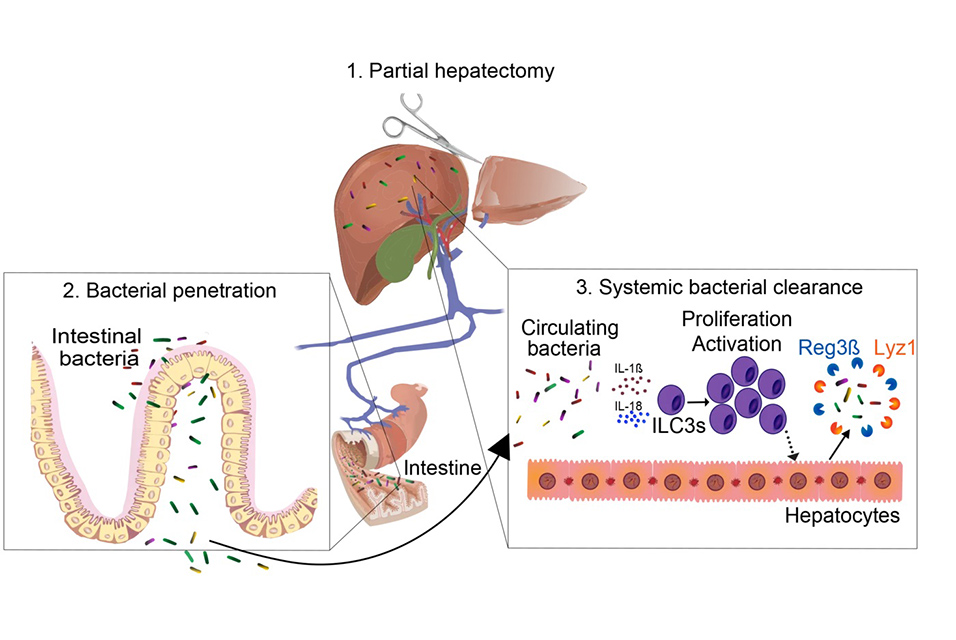
The pathogens seem to breach the intestinal barrier postoperatively and spread throughout the body via the bloodstream. These infections frequently occur after surgeries on the liver, pancreas, and bile ducts, as well as during operations on the small and large intestine. Patients who have undergone major liver resection, which involves removing large parts of the liver, are especially vulnerable to such infections, which significantly impede the healing process.
Crucial immune cells are present in the liver
The researchers then traced the infection control mechanisms in healthy patients. The liver plays a vital role in this process. "We know that unique immune cells residing in the liver are responsible for controlling these spreading bacteria and the healing process after major surgery," says Mercedes Gomez de Agüero, a junior research group leader in the Max Planck Research Group for Systems Immunology. They are a group of lymphocytes known as innate lymphoid cells (ILCs), which are crucial players in the innate immune system.
If bacteria from the intestine enter the liver through the bloodstream, these ILCs are activated and release specific messenger substances, such as interleukin 22, a protein that can trigger and regulate immune responses. In this manner, they induce liver cells to produce antimicrobial substances. "Innate lymphoid cells residing in the liver thus control the systemic spread of intestinal bacteria and effectively combat concomitant infections after surgery," she adds.
How can patients be protected from infections caused by their gut bacteria?
"Boosting immunity, therefore, represents a sensible prophylactic and therapeutic alternative strategy to the usual antimicrobial therapies to prevent concomitant infections after surgery," suggests Bern-based physician Guido Beldi. This approach should be considered until the factors responsible for gut bacteria penetrating the body's interior after surgical intervention have been identified. The research team intends to investigate this issue next.